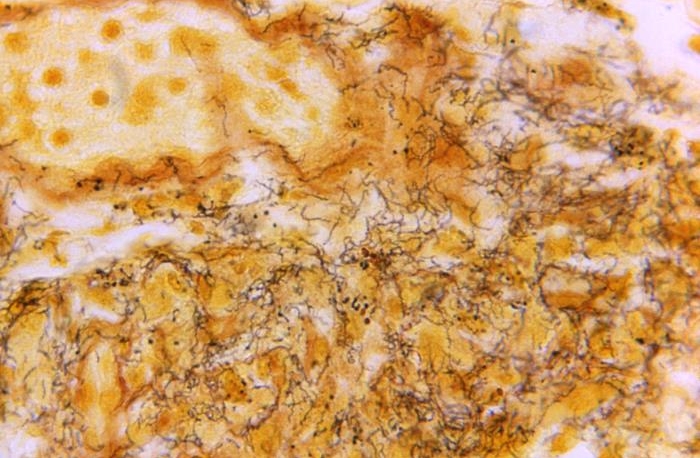
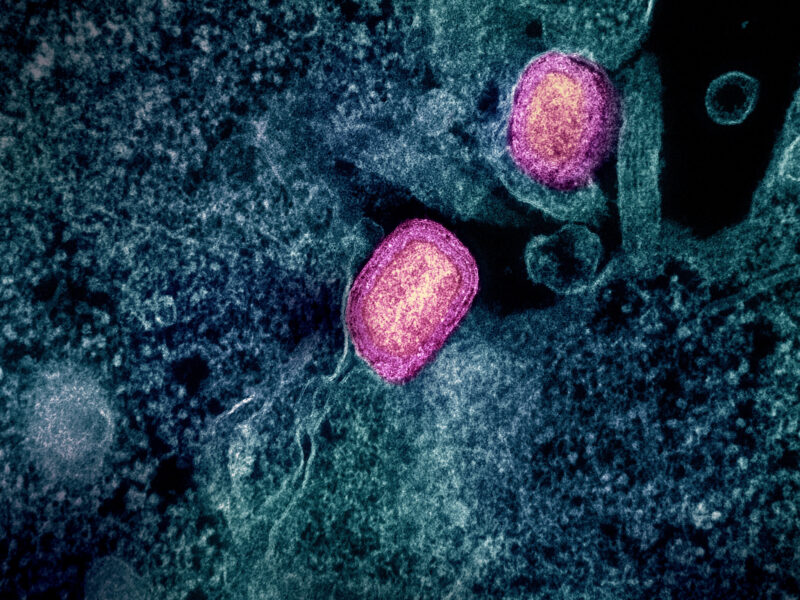
Image courtesy of CDC Public Health Image Library
On Monday, January 20th, the Nova Scotia Health Authority (NSHA) declared a province-wide outbreak of syphilis in Nova Scotia, Canada [1,2]. Syphilis cases used to be rare in Canada but since 2001, they have been increasing, particularly in urban areas, the male population, and in people over 30 [3]. The last outbreak occurred in the Halifax area only, starting in 2009, and peaking in 2013 with 84 cases [1,4]. Dr. Gaynor Watson-Creed, Nova Scotia’s Deputy Chief Medical Officer of health stated “We’re not really saying that any region of the province is particularly spared, which is different again than the 2013 outbreak that was largely in the city” [4]. Preliminary data records 82 cases in 2019, compared to 50 in 2018 and 38 in 2017 [1]. This is a 60% increase between 2018 and 2019 [4]. Cases are increasingly female, with approximately 20% of cases being female in 2019, compared to 10% in 2018, and 5% in 2017 [1]. The current outbreak is affecting people ages 20 to 65 [1]. These data align with patterns occurring in other parts of Canada [1]. In addition to syphilis, many sexually transmitted infections(STIs) are on the rise across Canada [4].
Syphilis is an STI primarily transmitted through oral, genital, or anal sex with an infected person [4]. Very rare forms of transmission include needle sharing, transmission via broken skin, or maternal transmission if a pregnant woman is infected [3]. Symptoms include open sores at the point of infection, flu-like illness, muscle pain and aches, fatigue, and rash presenting on the chest, back, palms, and bottom of feet [1]. Syphilis is referred to as “the great imitator” in the medical field as the symptoms are fairly general and broad, making syndromic diagnosis hard [3]. In addition to a wide-array of symptoms, the timing of symptom presentation varies by individual. On average, symptoms appear 21 days after infection, with a standard range of 10 to 90 days [1]. Some infected persons never present with symptoms [2]. Syphilis can be diagnosed via a blood test and is easily treated by penicillin, or other antibiotics, if caught early [1,3].
There are four stages of syphilis disease, with individuals being infectious, or able to spread the infection to others, during the primary and secondary phases [3]. The primary phase consists of the open sores at the point of exposure, and swollen glands in the groin area [3]. It is common for primary stage syphilis to go unnoticed by those infected [3]. The secondary phase of disease includes symptoms of patchy hair loss, rash on the soles of the feet, palms, or elsewhere on the body, fever, malaise, swollen glands, and sores in mouth and on the genitals [3]. The disease then moves into the latent phase [3]. If left untreated, the disease progress to the tertiary phase, which is severe and can result in damage to the brain, heart, other organs, blood vessels, and bones; this phase can also lead to death [1, 3].
As mentioned above, maternal transfer is also a concern with syphilis. If a pregnant woman has syphilis, it can be passed the fetus, which is known as congenital syphilis [1,3]. Congenital syphilis can result in birth defects, miscarriages, and stillbirths [1, 3]. The Public Health and Reproductive Care Program is recommending that doctors test pregnant patients twice for syphilis, once early in pregnancy, and again between 24 and 48 weeks [1]. To date, no cases of congenital syphilis have been reported in Nova Scotia [1].
Public health officials in Nova Scotia are working to slow and stop the outbreak through measures that have been successful in the past with other outbreaks. Dr. Watson-Creed stated “safer sex practices and getting tested for syphilis can help decrease the number of syphilis cases we are seeing in Nova Scotia currently… Knowing your status for sexually transmitted infections, including syphilis, is really important for our health and also the health of others” [1]. The previous outbreak was controlled via testing, and safe sex education campaigns [4]. Practicing safe sex includes using barrier protection, like condoms, getting tested yourself, and speaking with sexual partners, and potential partners about being tested. Those who test positive for syphilis should avoid unprotected sex until their antibiotic treatment is complete [3].
References
[2] https://globalnews.ca/news/6435355/syphilis-outbreak-nova-scotia-public-health/