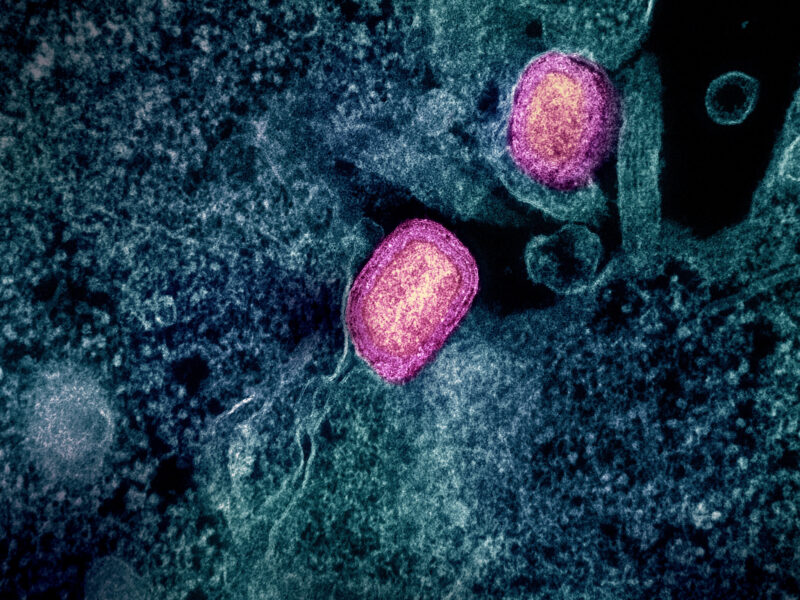
What began as a dip in a pool, ended in a leg amputation. According to a case report in the April 2012 Journal of Clinical Microbiology (JCM), a 14-year-old girl from Texas visited an urgent care facility late last year because of an enlarging bump on her leg (1). The bump presented itself after taking a swim in an algae-filled pool and, over the span of a few weeks, grew into a lesion that covered most of her leg.
Stephen J. Salipante of University of Washington Seattle, the lead author of the JCM report, stated that her initial treatment included antibiotic and antifungal regimens and aggressive surgical management, to no avail. With DNA sequencing, doctors discovered that the infection didn’t respond to antibiotics or antifungals because the infection was actually caused by Pythium insidiosum, which is an extremely rare, parasitic, fungus-like microorganism. The P. insidiosum had caused severe inflammation and extreme muscular necrosis in the patient's leg. To preserve the girl's life, all affected tissue needed to be removed, and her leg was amputated (1). She was discharged from the hospital after ten days, without antimicrobial therapy, and has shown no signs of infection since (1).
There is still much to learn about P. insidiosum. We do know that P. insidiosum typically affects horses and dogs. Only an approximate 150 human cases have been reported and most of them occurred in Thailand (as of 2010, 80% of documented cases were from Thailand (2)). However, because of its similarities to fungal infections, researchers assume that many cases go undiagnosed.
Salipante calls pythiosis, the condition caused by P. insidiosum, an emerging human pathogen and expects the number of cases to increase. Though the first cases of the disease were reported in horses in the late nineteenth century, pythiosis is “emerging” as it has been documented in a growing number of mammals since then. The first case of human pythiosis was reported in 1985 (1). As of 2010, human cases have been reported in Australia, New Zealand, Thailand, Malaysia, Brazil, Haiti, and the United States (2).
Species of the genus Pythium are extremely destructive to plant life and have caused serious economic losses in crop damage. P. insidiosum is the only known species to infect mammals. Sometimes referred to as “water mold,” because of its similarities to fungi the species only exists in wet environments and stagnant waters, and prefers tropical climates. Mammals are most often infected when in or near contaminated water bodies, though evidence from India shows the presence of the microbe inside a mosquito larva and suggests that it could be mosquito-borne as well (2). The fungus-like pathogen is attracted to wounds or small skin lesions by what is known as a “chemo-attractant.” Once inside the mammal via the lesion, the pathogen can invade surrounding tissue, causing severe inflammatory responses. In horses, the infection is usually in cutaneous (skin) tissues, manifesting in tumor-like masses or lesions. If the infection endures, it can reach the bone, causing lameness.
Dogs are also infected in the skin tissues though they usually suffer from infection in the gastrointestinal tract. Symptoms of infection include abdominal masses, stomach lesions, diarrhea, vomiting, depression, and weight loss.
Human pythiosis mostly occurs in the circulatory system, the eyes, or the skin. Symptoms vary depending on the severity and location of the infection (1). Morbidity and mortality rates in cases of human pythiosis are high (as of 2011, the mortality rate was 29 percent), because its rarity means that doctors lack familiarity with the infection. Further, successful treatment depends heavily on early detection, and this is a difficult infection to diagnose because of its similarities to fungal pathogens. Treatment of human pythiosis often means the removal of all affected tissues and limbs, though there is evidence of positive results in immunotherapy (injection of pythium insidiosum antigens). Interestingly, different species recognize different P. insidiosum antigens (the substance – usually protein or polysaccharide – that produces antibodies and an immune system response in the infected host). This means that immunotherapy will vary depending on the species being treated (2). The infection is not contagious; there is no evidence of human-to-human or animal-to-human transmission.
Wim Gaastra, lead author on an extensive overview of P. insidiosum wrote last year that there is still much to learn about its biology and how it affects humans. For the time being, “P. insidiosum will remain a fascinating microbe for those who study it and a devastating one for those who suffer from it” (2).
(1) Salipante, S. J., Hoogestraat, D. R., SenGupta, D. J., Murphy, D., Panayides, K., Hamilton, E., Castaneda-Sanechz, I., Kennedy, J. Monsaas, P.W., Mendonza, L., Stephens, K., Dunn, J.J., & Cookson, B.T. (2011). Molecular diagnosis of subcutaneous pythium insidiosum infection by use of pcr screening and dna sequencing. Journal of Clinical Microbiology, 50(4), 1480-1483.
(2) Gaastra, W., Lipman, L. J. A., De Cock, A. W. A. M., Exel, T. K., Pegge, R. B. G., Scheurwater, J., Vilela, R., & Mendoza, L. (2010). Pythium insidiosum: An overview. Veterinary Microbiology, 146, 1-16.